Corneal Edema
The cornea is a clear, transparent, dome-shaped structure that covers the front portion of the eye. An adult cornea is about 0.5 millimeters thick. It comprises five major layers, namely, epithelium (outer portion, having the ability to regenerate), Bowman’s membrane (hard, protective layer), stroma (thickest layer with collagen fibrils), Descemet’s membrane (thin layer) and endothelium (one-celled thick innermost layer). Since there are numerous nerve endings in the cornea, it is extremely sensitive.
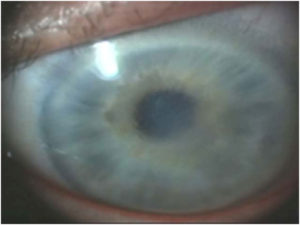 The cornea functions as a powerful refracting medium, contributing the maximum focusing power to the eyes. Cornea is kept transparent for the maximum vision clarity by supplying oxygen from the tears and pumping of water from the endothelium layer. When there is excess hydration or accumulation of fluid in the cornea portion, then it causes corneal swelling; a common eye problem referred to as corneal edema.
The cornea functions as a powerful refracting medium, contributing the maximum focusing power to the eyes. Cornea is kept transparent for the maximum vision clarity by supplying oxygen from the tears and pumping of water from the endothelium layer. When there is excess hydration or accumulation of fluid in the cornea portion, then it causes corneal swelling; a common eye problem referred to as corneal edema.
Causes and Symptoms of Corneal Edema:
Corneal edema is caused by the problems related to dehydration, viral infections, endothelial disorder, ocular surgery, traumatic injury, increased ocular pressure and at times, toxins. Among these, endothelial Fuch’s dystrophy is the most common cause of corneal edema. It is a hereditary disorder, characterized by slow and gradual loss of endothelial cells. Women are at a higher risk of endothelial dystrophy than men.
An infection by herpes viruses results in inflammatory responses in the cornea, leading to corneal edema. Corneal edema may also occur immediately or few years after the ocular surgery. It may occur due to impairment of endothelial layer by ultrasound radiation, damage of Descemet’s membrane and/or infusion of toxic medications in the cornea. In addition, strong topical and systemic medications can lead to corneal edema.
The most notable early symptoms of corneal edema are distorted or blurred vision: halos around lights, eye discomfort, photophobia (increased sensitivity to light) and sensitivity to foreign particles. Symptoms may progress to severe pain in the eye due to the corneal nerve damage. Pseudophakic bullous keratopathy (PBK) that results in the formation of fluid-filled bullae or blisters is commonly observed after the cataract surgery.
Diagnosis and Treatment of Corneal Edema:
As early symptoms of corneal edema are similar to cataracts, it is necessary to undergo ocular evaluation for the correct diagnosis of corneal edema. Doctors Mackman and Van Buren may conduct corneal topography or optical pachymetry (measurement of corneal thickness) in order to confirm the diagnosis.
The treatment of corneal edema varies based on the exact cause of the condition. In case of condition caused by ill-fitting or over wear of contact lenses, the use of correct contact lenses is recommended. Similarly, corneal edema caused by increased eye pressure is treated by lowering the pressure. Corneal edema developed as a post-surgery complication can be improved by administering eye drops prescribed by the eye care practitioner. The doctor may prescribe antibiotics and anti-inflammatory eye drops for the infection related corneal edema. In mild cases, corneal swelling is restricted to the epithelial layer and can be treated by using common salt solution. Salt solution (Muro 128 drops or ointment) extracts the excess fluid accumulation in the cornea by osmosis. In severe cases, corneal transplant (full or partial thickness) may be recommended as a treatment option.
At Phoenix Ophthalmologists, Dr. Van Buren can evaluate and treat ALL of the causes of corneal edema. Should you need surgery in the form of a full cornea transplant (penetrating keratoplasty) or a partial transplant (descement stripping endothelial keratoplasty or DSEK).
